A new study of over 20,000 U.S. adults finds that a healthier diet and increased exercise lead to weight loss that lowers the risk of heart disease, while skipping meals and taking prescription diet pills lead to minimal weight loss, weight maintenance, or weight gain.
However, for many in the study sample, losing a “clinically significant” 5% of their body weight did not eliminate their risk factors for cardiovascular disease, according to the findings. In fact, regardless of reported weight changes, the average composite score on eight risk factors for heart disease was the same across the entire study population.
The study is the first to compare weight-loss strategies and outcomes in the context of the American Heart Association’s “Life’s Essential 8,” a checklist that promotes heart disease risk reduction by pursuing recommended metrics for body weight, blood pressure, cholesterol, blood sugar, smoking, physical activity, diet, and sleep. The AHA first defined cardiovascular health with “Life’s Simple 7” metrics in 2010, and the recommendations were updated to “Life’s Essential 8” in June 2022.
Clinically significant weight loss results in improvements in some health indice. People should feel hopeful in knowing that losing just 5% of their body weight is meaningful in terms of clinical improvements.
Colleen Spees
The researchers from Ohio State University discovered that overall, U.S. adults scored 60 out of 100 on the eight measures, indicating that there is still room for improvement even among those whose diet and exercise habits helped move the needle on some metrics.
“The Life’s Essential 8 is a valuable tool that provides the core components for cardiovascular health, many of which are modifiable through behavior change,” said senior study author Colleen Spees, associate professor of medical dietetics at Ohio State.
“Based on the findings in this study, we have a lot of work to do as a country,” she said. “Even though there were significant differences on several parameters between the groups, the fact remains that as a whole, adults in this country are not adopting the Life’s Essential 8 behaviors that are directly correlated with heart health.”
The research was published recently in the Journal of the American Heart Association.
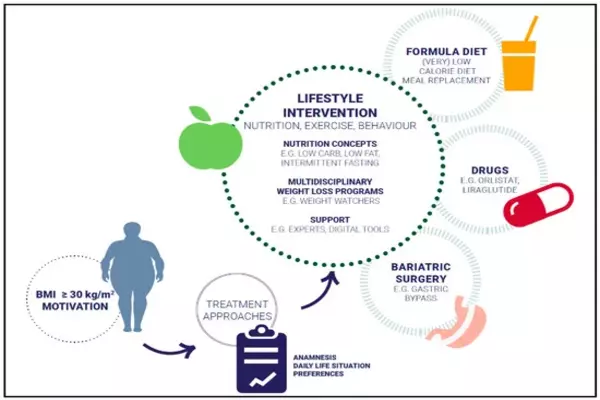
Behavior patterns of people who achieve clinically significant weight loss
The study used data from 20,305 U.S. adults aged 19 and up (average age 47) who took part in the National Health and Nutrition Examination Survey (NHANES) between 2007 and 2016. Participants provided information about their smoking status, physical activity, average number of hours of sleep per night, weight history and weight loss strategy, and what they had eaten in the previous 24 hours. Body mass index, blood pressure, LDL (bad) cholesterol, and blood glucose levels were all measured during physicals and lab tests.
The data was used by the Ohio State researchers to determine individuals’ values for Life’s Essential 8 metrics and to assess their diet quality using the Healthy Eating Index, which measures adherence to the U.S. Dietary Guidelines for Americans.
Within the sample, 17,465 individuals had lost less than 5% of their body weight, maintained their weight or gained weight in the past year. The other 2,840 reported intentional loss of at least 5% of their body weight in the same time frame.
“Clinically significant weight loss results in improvements in some health indices,” Spees said. “People should feel hopeful in knowing that losing just 5% of their body weight is meaningful in terms of clinical improvements. This is not a huge weight loss. It’s achievable for most, and I would hope that incentives people instead of being paralyzed with a fear of failure.”
In this study, adults who lost clinically significant weight reported higher diet quality, including higher intakes of protein, refined grains, and added sugar, as well as more moderate and vigorous physical activity and lower LDL cholesterol than the control group. The weight-loss group, on the other hand, had a higher average BMI and HbA1c blood sugar measure, as well as fewer hours of sleep – all of which would lower their composite Life’s Essential 8 score.
People who did not lose at least 5% of their body weight were more likely to skip meals or use prescription diet pills as weight-loss strategies. This group also reported using low-carb and liquid diets, taking laxatives or vomiting, and smoking.
“We saw that people are still gravitating to non-evidence-based approaches for weight loss, which are not sustainable. What is sustainable is changing behaviors and eating patterns,” Spees said.
With federal data predicting that more than 85% of the adult U.S. population will be overweight or obese by 2030 (up from 73% now), Spees believes that a paradigm shift toward prevention is required to avert related increases in heart disease and other health problems.
“We absolutely must shift toward disease prevention rather than waiting until people are diagnosed with a disease.” This becomes quite overwhelming, and people may believe it is too late at that point,” she explained.
Prescriptions for regular visits with registered dietitians trained in behavior change, complete with insurance reimbursement – similar to physical therapy, she suggested.