Pfizer and Moderna’s mRNA COVID-19 vaccines continue to save lives. Yet another paper distributed in the journal Immunizations gives proof that the two antibodies are not comparable with regards to safeguarding more seasoned adults against death.
For individuals ages 60+ who got just the underlying two dosages and no promoter portion, the risk of death from coronavirus for Pfizer vaccinees was generally 2.5 times higher than the risk for Moderna vaccinees. From April 2021 to June 2022, the study period, a higher risk was observed. There were no differences in the effectiveness of the vaccine after two doses for younger people or the 60+ group after a booster dose.
Senior author Bernard Black, a health policy researcher at Northwestern’s Pritzker School of Law, stated, “We need more refined messaging around boosters that explains who stands to benefit the most and targets those people.” He added, “Supporters are vitally significant for Pfizer vaccinees. It is necessary to convey that message. It is unacceptable for our public health agencies to continue acting as if all COVID vaccines are roughly equivalent.”
“Boosters are critical for Pfizer vaccinees. That message must be conveyed. Our public health agencies should stop acting as though all COVID vaccines are the same.”
Senior author Bernard Black, a professor of law at Northwestern’s Pritzker School of Law.
Important selection effects are also highlighted in the study, which measured vaccine protection against death but not against hospitalization or other outcomes. Those who were vaccinated were healthier than those who were not. Collectively, they were less inclined to bite the dust for different reasons, and in this way, they were less inclined to pass on the coronavirus even had they not been immunized. Besides, among individuals who were immunized, Pfizer vaccinees aged 60+ were more grounded than Moderna vaccinees.
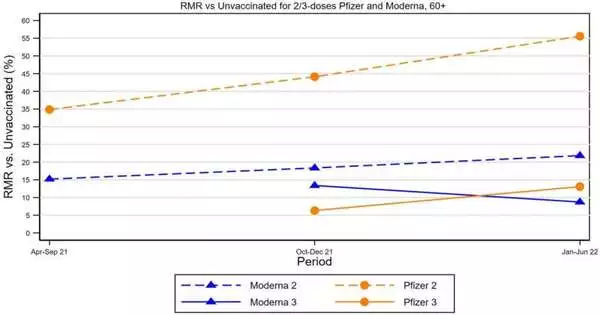
Controlling for these determination impacts, the two immunizations still altogether decreased mortality; however, in the omicron period, the leftover mortality risk compared with unvaccinated individuals was 57% for two-portion Pfizer vaccinees age 60+, compared with just 23% for Moderna vaccinees.
For instance, if a 60-plus person who was not vaccinated had a risk of 1 percent of dying from COVID-19 (based on their age, gender, health, and other personal characteristics), the same person would have a chance of death of 0.57 percent if they took two doses of Pfizer (a 43 percent reduction in risk) and a chance of death of 0.23 percent if they took two doses of Moderna (77% reduction in risk).
For both vaccines, a booster dose would reduce the remaining risk to approximately 1%. Furthermore, for booster recipients, the effectiveness disparity between Moderna and Pfizer vanished.
Therefore, everyone over the age of 60 should get a booster shot, but Pfizer vaccine recipients especially need them. The fact that the Moderna vaccine contains a dose that is significantly higher than the Pfizer vaccine’s (100 g versus 30 g) may account for this difference. In order to prime their immune systems, older bodies may require a stronger kick from a larger dose of Moderna.
Two-dose vaccine recipients had almost no deaths among people between the ages of 18 and 49. There was no evidence of a difference in effectiveness between Pfizer and Moderna, but there were a significant number of deaths among people between the ages of 50 and 59, making a booster dose necessary.
In aggregate, promoter security is exceptionally significant for more established individuals aged 60+, particularly Pfizer immunizations; it has a lot of value for people in their 50s but only a little for younger people, for whom the first two doses still do a lot to prevent death.
Notwithstanding Dark, the group included different analysts partnered with Northwestern College, the Clinical School of Wisconsin, and William and Mary. For their analysis, the authors used a dataset of linked mortality and vaccination records for all adults in Milwaukee County, Wisconsin (722,000 adults) from January 1, 2021, to June 30, 2022.
Their review is quick to control for the propensity of individuals who got the Pfizer immunization to be more grounded than the people who got the Moderna antibody (to some extent in Milwaukee, the region that the creators contemplated).
The COVID Excess Mortality Percentage (CEMP)—the percentage increase in mortality risk due to COVID in comparison to the risk from other natural causes—was the primary metric that the authors investigated. CEMP is calculated by dividing the mortality from non-COVID natural causes for a given group by the mortality from COVID-19 for that group.
More information: Vladimir Atanasov et al, Selection Effects and COVID-19 Mortality Risk after Pfizer vs. Moderna Vaccination: Evidence from Linked Mortality and Vaccination Records, Vaccines (2023). DOI: 10.3390/vaccines11050971