Scientists have shown that modifying an enzyme produced by the anthrax-causing bacterium can protect mice from infection with the deadly disease. Their findings, which were published today in the online edition of Science Translational Medicine, point to a potential therapeutic strategy for treating multidrug-resistant strains of anthrax and could lead to new treatments for other bacterial infections.
Bacillus anthracis causes anthrax, an acute disease. Some animal species are more resistant to anthrax infection than others. This trait has been linked to the severity of the local inflammatory response, implying that in nonimmunized hosts, innate immunity is the first line of defense against B. anthracis infection.
Bacillus anthracis, the bacterium that causes anthrax, is widely regarded as one of the most serious bioterrorism threats, as well as a public health issue in many parts of the world. Its ability to cause disease is due to three main components: lethal toxin, edema toxin, and capsule. The researchers devised a method to degrade the capsule surrounding the bacterium, allowing it to be ingested and destroyed by white blood cells, thereby reducing virulence.
The discovery of the capsule depolymerase enzyme within the anthrax bacillus prompted us to try to use that enzyme to remove the capsule. Once this was proven to be successful, we used recombinant DNA technology and protein engineering methods to engineer and reconfigure the enzyme in novel ways.
Arthur M. Friedlander
According to the paper’s senior author, Arthur M. Friedlander, M.D., public health officials have become increasingly concerned about anthrax strains that appear to be resistant to treatment with known antibiotics. He and his colleagues at the United States Army Medical Research Institute of Infectious Diseases (USAMRIID) collaborated with researchers from the United States Naval Research Laboratories, the University of Washington in Seattle, and the University of California at Davis to investigate alternative treatment approaches that do not rely on antibiotics.
One promising approach would be to make the bacterium more susceptible to the innate immune system, which is the human body’s first line of defense against a pathogenic “invader.” The innate immune response is made up of physical, chemical, and cellular defenses that work to prevent the spread of foreign pathogens throughout the body right away. Capsular depolymerases, which are naturally produced by several types of bacteria, have emerged as a potential new class of antivirulence agents.
“The discovery of the capsule depolymerase enzyme within the anthrax bacillus prompted us to try to use that enzyme to remove the capsule,” Friedlander explained. “Once this was proven to be successful, we used recombinant DNA technology and protein engineering methods to engineer and reconfigure the enzyme in novel ways.”
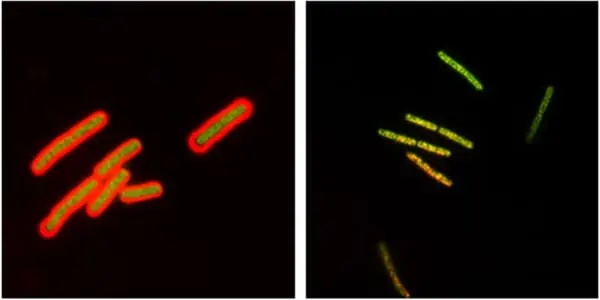
Circular permutation by protein design was used to improve stability and make the enzyme easier to produce, and pegylation was used to improve the enzyme’s pharmacokinetics – the properties that allow it to be absorbed and distributed properly within the body. The pegylated enzyme, known as PEG-CapD-CPS334C, was then tested to ensure it retained its enzymatic activity.
In the study, PEG-CapD-CPS334C completely protected 10 of 10 mice infected with anthrax spores from a nontoxigenic encapsulated strain, while only 1 of 10 mice receiving a control treatment survived. Similarly, PEG-CapD-CPS334C treatment of mice infected with a fully virulent encapsulated strain saved 8 of 10 animals, while only 2 of 10 control animals survived.
“This strategy makes B. anthracis susceptible to innate immune responses while avoiding the use of antibiotics,” the authors concluded. “These findings imply that enzyme-catalyzed capsule removal could be a potential therapeutic strategy for the treatment of multidrug-resistant anthrax and other bacterial infections.”
It may also allow Warfighters exposed to anthrax through natural or other means to be treated at the time of exposure or shortly afterwards, preserving combat power in forward areas where advanced diagnostics and treatments may be unavailable.
Bacillus anthracis, the anthrax etiological agent, infects mammals. Upon entry into the host, the spore, the infective form of B. anthracis, germinates and gives rise to the vegetative form that produces the virulence factors, mainly the edema and lethal toxins and the capsule. In the absence of treatment, the expression of these factors results in anthrax, a combination of toxemia and rapidly spreading infection that evolves into septicemia with a fatal outcome. Some animal species are more resistant to anthrax infection than others.