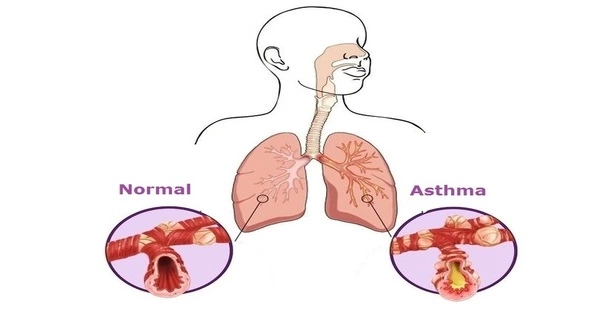
Several studies have revealed a relationship between childhood food allergies and an increased risk of developing asthma. Children who have food allergies are more likely to develop asthma symptoms such as wheezing, coughing, and shortness of breath. According to a world-first study, having a food allergy as a baby is connected to asthma and impaired lung function later in childhood.
The study, coordinated by Murdoch Children’s Research Institute and published in the Lancet Child & Adolescent Health, discovered that early childhood food allergy was related with an increased risk of both asthma and decreased lung growth by the age of six.
According to Associate Professor Rachel Peters of Murdoch Children’s Research Institute, this is the first study to look at the link between challenge-confirmed food allergy in infancy and asthma and poorer lung health later in childhood.
Lung development is related to a child’s height and weight, and children with food allergies may be shorter and lighter than their peers who do not have allergies. This could explain the relationship between food allergies and lung function.
Asso. Prof. Rachel Peters
The Melbourne study included 5276 infants from the HealthNuts project who were subjected to skin prick testing for common food allergens such as peanut and egg, as well as oral meal challenges to screen for food allergy. Children were given additional food allergy and lung function testing when they were six years old.
The study discovered that by the age of six, 13.7% of children had been diagnosed with asthma. When compared to children without a food allergy, babies with a food allergy were nearly four times more likely to develop asthma at six years of age. The effect was greatest in children who had a food allergy that lasted until the age of six, as opposed to those who had outgrown their allergy. Children with food allergies have a higher risk of having poor lung function.
Food allergy in infancy, whether resolved or not, was connected to poorer respiratory outcomes in children, according to Associate Professor Peters.
“This association is concerning because reduced lung growth in childhood is associated with health problems in adulthood, including respiratory and heart conditions,” she said.
“Lung development is related to a child’s height and weight, and children with food allergies may be shorter and lighter than their peers who do not have allergies. This could explain the relationship between food allergies and lung function. Both food allergy and asthma are caused by comparable immunological responses. The development of infants with food allergies should be watched. We recommend children who are avoiding foods due to allergies to be under the care of a dietitian so that nutrition can be catered for to promote good growth.”
Food allergy affects 10 percent of babies and 5 percent of children and adolescents. Suba Slater’s, son Zane, 15, is allergic to eggs, sesame and peanuts and has asthma.
“As a newborn, he developed eczema on his back, and I assumed it was caused by something in my diet because I was breastfeeding,” she explained. “We took him to the hospital for tests, and the multiple food allergies were confirmed.”
Suba stated that she was not well versed in the connection between food allergies and asthma prior to Zane’s diagnosis.
“Because our eldest child also has allergies, we were very focused and vigilant about the food allergy aspect,” she explained. It is critical to demonstrate this link through study and to make parents and medical professionals aware of it. We didn’t know to be on the watch for asthma once we realized Zane had food allergies, and it wasn’t on our radar.
“Looking back, he most likely had asthma long before we could hear that he was struggling with his breathing. If we had been aware of the association we would have sought medical help much sooner.”
Suba said Zane had participated in several food challenges at the Murdoch Children’s but his asthma had complicated his participation at times.
“By participating in the food challenges, we discovered that Zane is now much more tolerant of egg in baked goods and certain nuts and has learned how to incorporate these foods into his diet,” she explained. “However, before attempting a challenge, he must first undergo a spirometry test to ensure that his lung function is optimal in case the allergenic food triggers his asthma.” He has missed visits because his lungs aren’t strong enough.”
Professor Shyamali Dharmage of Murdoch Children’s Hospital and the University of Melbourne said the findings would assist clinicians personalize patient care and promote more vigilance in monitoring respiratory health. Children with a food allergy should be managed by a clinical immunology or allergy specialist for ongoing management and education.