A group from the College of Michigan Rogel Disease Center and School of Dentistry, led by Yu Leo Lei, D.D.S., Ph.D., has distinguished a component in mice for what stoutness means for an oral tumor’s capacity to escape from the resistant framework.
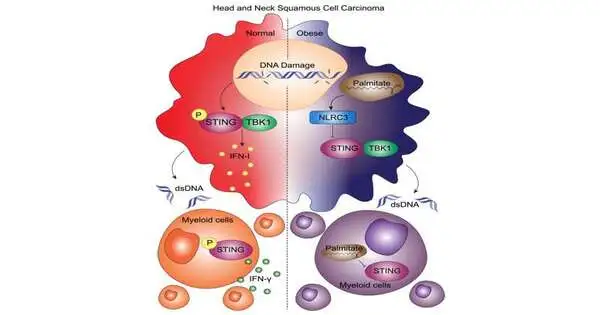
Obesity contributes to the creation of a type of tumor microenvironment that encourages tumor progression, according to this study, which was published in Cell Reports. How precisely this happens lies in the connection between the soaked unsaturated fats, the STING-type-I interferon pathway, and NLRC3.
“When it comes to obesity, we tend to think about the increased risks for gastrointestinal tumors, breast cancer, pancreatic cancer, and ovarian cancer. Multiple recent prospective cohorts encompassing millions of people from different continents demonstrated a previously unknown relationship between obesity and the risk of mouth cancer.”
Lei, a pathologist-immunologist and lead author of this study.
“When it comes to obesity, we tend to think about the increased risks for gastrointestinal tumors, breast cancer, pancreatic cancer, and ovarian cancer,” said Lei, the study’s lead author and pathologist-immunologist. A previously unrecognized link between obesity and the risk of oral cancer was discovered by multiple recent prospective cohorts involving millions of people from several continents.”
“Myeloid cells in stout mice were harsh toward STING agonists and were more suppressive of lymphocyte enactment compared with the myeloid cells from inclines,” made sense to Lei. In the tumor microenvironment, this feature caused the loss of immune subsets that were necessary for anti-tumor immunity.
The group found that soaking unsaturated fats can hinder the STING pathway, which is prompted by cytosolic DNA and advances antigen-introducing cell development, by inciting a protein called NLRC3.
According to Lei, this is the first study to establish a mechanistic link between oral cancer immune escape and obesity. “The translational implications are exciting to us,” he went on to say.
Cancer patients frequently have obesity as a co-morbidity. In two recent studies, patients with oral cancer who were taking statins, cholesterol-lowering medications, had better overall and cancer-specific survival. This study lays out a robotic connection for those perceptions and features the capability of focusing on unsaturated fat digestion in renovating the host against cancer-resistant reactions,” said Lei.
For improved oral cancer prevention in high-risk individuals, Lei’s team will next investigate how obesity regulates other immune-activating pathways and identify novel intervention targets. Before this can move to the clinic, more work needs to be done.
Extra review creators incorporate Blake Heath, Ph.D.; researcher at the School of Dentistry, Wang Gong; and Hülya Taner, D.D.S., Ph.D. Candidate D.
More information: Blake R. Heath et al, Saturated fatty acids dampen the immunogenicity of cancer by suppressing STING, Cell Reports (2023). DOI: 10.1016/j.celrep.2023.112303