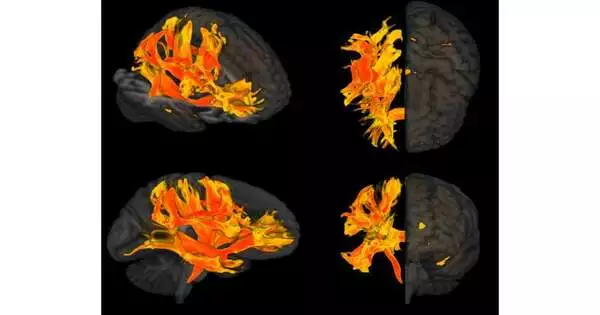
Researchers have discovered for the first time which brain regions are damaged by high blood pressure and may play a role in mental decline and the development of dementia.
It is known that high blood pressure plays a role in the development of dementia and the impairment of brain function. This is demonstrated by the study, which was recently published in the European Heart Journal. It assembled data from a blend of attractive reverberation imaging (X-ray) of minds, hereditary examinations, and observational information from a great many patients to take a gander at the impact of hypertension on mental capability. After that, the findings were checked on a separate large group of patients in Italy.
“By using this combination of imaging, genetic, and observational approaches, we have identified specific parts of the brain that are affected by increases in blood pressure, including areas called the putamen and specific white matter regions,” said Tomasz Guzik, Professor of Cardiovascular Medicine at the University of Edinburgh (UK) and Jagiellonian University Medical College, Krakow (Poland), who led the research. We thought that high blood pressure might have an effect on memory loss, thinking skills, and dementia in these areas. When we checked our findings by studying a group of high-blood-pressure patients in Italy, we discovered that the identified brain regions were affected.
“We hope that our findings will assist us in developing novel treatments for high blood pressure patients with cognitive impairment. We might be able to learn more about how high blood pressure affects the brain and causes cognitive problems by studying the genes and proteins in these brain structures. In addition, we may be able to predict who will develop memory loss and dementia more quickly in the context of high blood pressure by looking at these particular brain regions. With precision medicine, we might be able to target more intensive treatments to prevent cognitive impairment in patients who are most at risk.
“For the first time, we discovered particular brain regions that may be directly linked to high blood pressure and cognitive impairment. This was made feasible by the availability of data from the UK Biobank, including MRI brain pictures, as well as prior research that identified genetic variations that alter the structure and function of over 3000 brain areas.”
Associate Professor Mateusz Siedlinski, also a researcher at Jagiellonian University Medical College,
Thirty percent of people worldwide have high blood pressure, and another thirty percent are in the early stages of the condition. It has been demonstrated in studies to have a long-term impact and an impact on brain function. However, the precise mechanisms by which high blood pressure harms the brain and which specific regions are affected were unknown up until this point.
To see if high blood pressure was actually the cause of changes to specific parts of the brain rather than just being associated with these changes, Prof. Guzik and an international team of researchers used brain MRI imaging data from over 30,000 participants in the UK Biobank study, genetic information from genome-wide association studies (GWAS) from UK Biobank and two other international groups (COGENT and the International Consortium for Blood Pressure), and a method called Mendelian randomization.
Prof. Guzik stated, “Mendelian randomization is a method of using genetic information to understand how one thing affects another.” In particular, it determines whether the effect is just a coincidence or if something is potentially causing it. It works by looking at a person’s genetic information to see if there is a link between the genes that make you more likely to have high blood pressure and the results. High blood pressure is more likely to be the cause of the situation if there is a relationship. This is due to the random transmission of genes from parents, which prevents them from being influenced by other factors that could muddle the results. According to our research, “high blood pressure might really be causing brain dysfunction at that location, leading to problems with memory, thinking, and dementia.” If a gene that causes high blood pressure is also linked to specific brain structures and their function, then this suggests that high blood pressure is the cause of dementia.”
Higher blood pressure and diminished cognitive function were linked to changes in nine brain regions, the researchers discovered. These included the putamen, a spherical structure in the front of the brain that is in charge of controlling movement and influencing a variety of learning styles. The anterior thalamic radiation, anterior corona radiata, and anterior limb of the internal capsule—white matter regions that connect and enable signaling between various brain regions—were the other affected areas. The front thalamic radiation is engaged with leader capabilities, like the preparation of basic and complex day-to-day undertakings, while the other two locales are engaged with direction and the administration of feelings.
Changes in measures of brain activity, changes in connections between various parts of the brain, and reductions in brain volume and surface area on the brain cortex are examples of these changes.
“Our study has, for the first time, identified specific places in the brain that are potentially causally associated with high blood pressure and cognitive impairment,” said Associate Professor Mateusz Siedlinski, the study’s first author and researcher at Jagiellonian University Medical College. This was made possible in a unique way because of the availability of data from the UK Biobank, including MRI brain images, and previous research that identified genetic variants that affect the structure and function of over 3000 brain regions.”
“It has been known for a long time that high blood pressure is a risk factor for cognitive decline,” said co-author Professor Joanna Wardlaw, Head of Neuroimaging Sciences at the University of Edinburgh. “How high blood pressure damages the brain was not clear.” This study demonstrates that certain brain regions are particularly susceptible to blood pressure damage, which may aid in the identification of individuals at risk for cognitive decline in its earliest stages and potentially enable more effective therapies in the future.
The fact that most of the people who took part in the UK Biobank study were white and middle-aged makes it difficult to extrapolate the results to older people.
A companion publication is composed by Dr. Ernesto Schiffrin, from the Sir Mortimer B. Davis-Jewish General Clinic and McGill College, Montreal (Canada), and Dr. James Engert, from the McGill College Wellbeing Center Exploration Foundation, Montreal. “Further mechanistic studies of the effects of BP [blood pressure] on cognitive function are required to determine precise causal pathways and relevant brain regions,” they point out.
Additionally, they emphasize one of the study’s findings regarding systolic and diastolic blood pressure (SBP and DBP): The possibility of distinct causal effects between SBP and DBP is perhaps one of this study’s more intriguing findings. When SBP and DBP were analyzed separately, the authors discovered some results for cognitive function that overlapped. In any case, when every boundary is examined in the wake of adapting to the next, or in multivariable models, captivating discoveries start to arise. When adjusted for SBP, DBP actually protects against cognitive decline when taken on its own. They write, “This result was true both when observed and when using Mendelian randomization,” and they go on to discuss the potential causes of this.
More information: Tomasz J Guzik et al, Genetic analyses identify brain structures related to cognitive impairment associated with elevated blood pressure, European Heart Journal (2023). DOI: 10.1093/eurheartj/ehad101
Ernesto L. Schiffrin et al, Hypertension, brain imaging phenotypes and cognitive impairment: lessons from Mendelian randomisation, European Heart Journal (2023). DOI: 10.1093/eurheartj/ehad187