According to a study published April 19 in the open-access journal PLOS Medicine, children’s cognitive development may be impaired regardless of whether biological parent has type 1 diabetes. For the first time, the study found that having a parent with a chronic disease, such as type 1 diabetes, is connected with lower school achievement rather than maternal high blood sugar during fetal development.
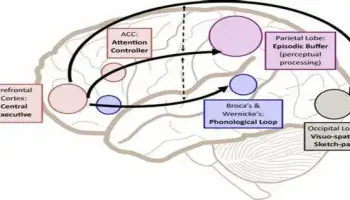
The severity of CD in type 1 diabetes was found to be affected by the age of onset and duration, as well as the existence of proliferative retinopathy and autonomic neuropathy in a number of investigations. The diabetes-related CD has been found in children and adolescents as well as adults. The majority of neuroimaging investigations of type 1 diabetes patients found no abnormalities in whole-brain volumes; however, they did find specific deficits in gray matter volume or density within the frontal, posterior, and temporal cortex, as well as subcortical gray matter. Diffusion tensor imaging studies on middle-aged persons with long-standing type 1 diabetes revealed partial lesions in the white matter and decreased fractional anisotropy in posterior brain areas.
The impact of maternal diabetes during pregnancy on the cognition of their children has received a lot of attention. Glucose crosses the placenta, and maternal hyperglycemia, or high blood sugar, can damage fetal development, particularly the baby’s brain. There is minimal research on different types of diabetes and the impact of having a father with type 1 diabetes.
Lower test scores in children of type 1 diabetes moms appear to reflect a negative connection with having a parent with type 1 diabetes rather than a specific harmful effect of maternal type 1 diabetes during pregnancy on the fetus. This was demonstrated in a recent large Danish cohort research involving 622,073 children.
Anne Laerke Spangmose
Anne Laerke Spangmose and colleagues from Copenhagen University Hospital in Denmark gathered information from Danish registrations as well as test results in arithmetic for grades three and six, and reading for grades two, four, six, and eight. Over a seven-year span, the team included 622,073 youngsters aged 6 to 18 who attended public schools. There were 2,144 children with type 1 diabetes in their mothers, 3,474 children with type 1 diabetes in their fathers, and 616,455 children in the general population. Children of type 1 diabetes moms and fathers had mean scores of 54.2 and 54.4, respectively, compared to mean scores of 56.4 in the general population.
Diabetes can have an impact on a child’s learning since it can impair attention, memory, processing speed, and perceptual skills if not handled properly. It is critical that a child is supported at school so that they can manage their diabetes and get the most out of their education.

Some students with diabetes will have more absences than others. This will not be the case for every child with diabetes, but if they need to take time off for hospital appointments or because they are ill as a result of diabetes, it is critical that they be not penalized for it.
It is the parent’s job to notify you as soon as possible that their child has diabetes, so make sure you discuss your school’s absence policy with them and how you can be flexible to ensure the child does not feel set up to fail.
The team acknowledges that having a parent with a major chronic disease, such as diabetes, might cause stress and harm a child’s academic performance. However, this study indicates a new reason for previously known deleterious effects of maternal type 1 diabetes on children’s cognitive development during pregnancy.
Spangmose continues, “Lower test scores in children of type 1 diabetes moms appear to reflect a negative connection with having a parent with type 1 diabetes rather than a specific harmful effect of maternal type 1 diabetes during pregnancy on the fetus. This was demonstrated in a recent large Danish cohort research involving 622,073 children.”
Higher CD rates and faster progression in type 1 diabetes can be explained by the direct impact of altered glucose metabolism on the brain as well as diabetes-related cardiovascular disease. Because the existence and progression of CD dramatically reduces the quality of life of diabetic patients, more multidisciplinary research including recent advances in neuroimaging and type 1 diabetes therapy are needed to examine this issue.